Health x Wellness
Taking care of your prostate
This is part two of a series contributed by Dr. Jay Lim, a urologist about prostate cancer. Part 1 can be found here.
Before we dive into the topic of taking care of your prostate, it is vital to acknowledge the elephant in the room, i.e. “Can Prostate Cancer be prevented at all?”
According to the professional bible that most Urologists in Singapore refer to, the European Association of Urology (EAU) guideline states that “No conclusive data exist which could support specific preventive or dietary measures aimed at reducing the risk of developing Prostate Cancer.”.
Certain genetic factors are associated with the risk of aggressive Prostate Cancer, and it is best to speak to your Urologist if you have a family member who has aggressive prostate cancer in their 50s or younger.
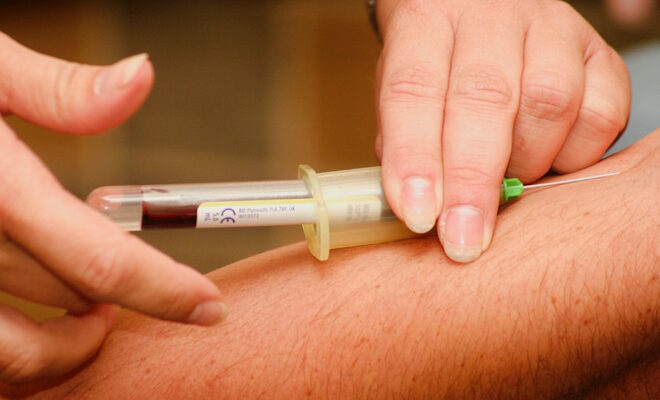
For the rest, there are a few ways to monitor the health of your prostate. The most common way of screening is through Prostate Specific Antigen test. PSA is a blood test that measures the level of Prostate Specific Antigen in your body. PSA is a protein that is secreted by both normal and abnormal prostate cells. This blood test is commonly performed as part of health screening packages in the appropriate age group. It is easily performed as it does not require fasting.
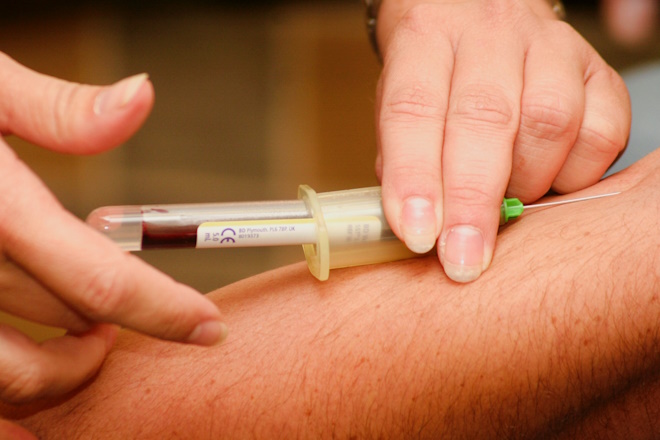
PSA can be elevated in BPH, prostatitis and prostate cancer. There is no normal level of PSA as it is a progress measurement of risk; however, 4.0ng/dl is generally accepted as the cutoff between normal and abnormal. An important point to highlight here is that while most commercial labs will highlight values above 4.0ng/dl as red or abnormal, it is not to say that you have prostate cancer, as PSA is a measurement of risk. Similarly, a value of 3.9ng/dl does not guarantee no prostate cancer too. While you may argue that it is a rudimentary interpretation of the cancer marker test for prostate cancer, it is the best (and most established) screening tool we have.
Thankfully, PSA is not the only tool that Urologists depend on to assess your prostate cancer!
We employ an even more rudimentary (but time-tested) method to screen for prostate cancer. Unfortunately, due to its location, the prostate is most accessible via the rectum, and DRE is an established component of annual physical examinations for men at risk for prostate cancer. Digital Rectal Examination (DRE) is the most often talked about the part after a visit to the Urologist amongst Singaporean men at the coffee shop and void decks. Some wear it as a badge of honour as the uninitiated cringe while their peers describe the process. This examination is subjected to individual interpretation and is a helpful adjunct if performed by an experienced Urologist.
If your Urologist decides, based on your PSA, DRE and medical history, that there is a risk of prostate cancer, we proceed to the next step of surviving your prostate, which is to perform a prostate biopsy.
A prostate biopsy confirms the presence of prostate cancer and the grade of the cancer (benign sheep vs dangerous wolf).
There are a variety of ways that the prostate can be sampled. In many parts of the world, the prostate is still sampled with a needle via the rectum. A needle is passed through around 12 to 18 times to get prostatic tissue for testing under local anaesthetic. As can be imagined, this route is associated with a risk of sepsis or severe infection due to the presence of stool in the rectum. Apart from infection, trans-rectal ultrasound-guided (TRUS) biopsy is a random process that can miss small cancers as the Urologist is guided by the black-and-white pictures of an ultrasound that does not tell you where the cancer is located.
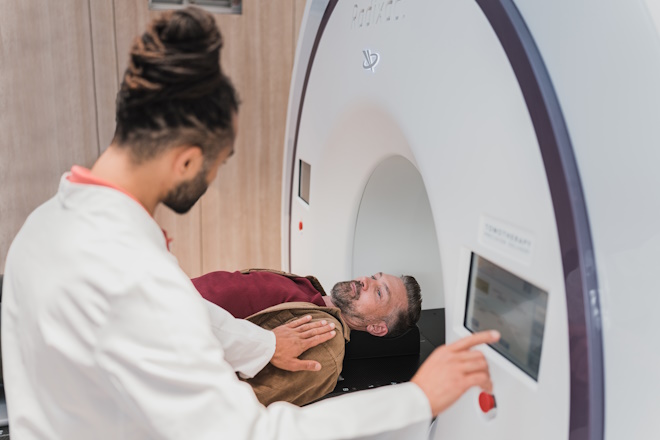
In recent years, there has been a move toward image-guided biopsy of the prostate. Before any biopsy, Magnetic Resonance Imaging (MRI) of the prostate is performed as the first step. MRI prostate grade regions within the prostate using the PIRADs 3-5 grading. The higher the grade, the more likely the presence of abnormality within the specific region.
Imagine going into battle without knowing where the enemy is and carpet bombing mindlessly in the general direction. With an MRI prostate as a guide, we know where the enemy is and can attack a particular region specifically.
There are a variety of imaging-guided prostate biopsy platforms regularly in use, as we do not use TRUS-guided biopsy in private hospitals.
I prefer the Biobot platform, which was developed locally by my alma mater, Singapore General Hospital, for which I have direct access to the engineers locally. This MRI-guided robotic system allows me to plan my biopsy purposefully. It is simple to use and will enable me to get to within 1-2mm of my intended target due to experience. Most importantly, the biopsy needle for this platform goes through the skin instead of the rectum and makes two little holes on either side of the perineum. Whether it is 10 or 20 biopsies, you only need a single puncture on the skin, which is dressed with a simple plaster. Minimal infection risk, targeted biopsies and many more areas of the prostate is sampled as you can take up to 50 cores under General Anesthetic, which reduces missed lesions.
As the biopsy is performed as a day procedure, you will be discharged home on the same day!
The biopsy is processed, and results are usually available after a week. Our Pathologist colleagues will review the biopsy and give an all-clear or score your prostate cancer between 6 and 10, which indicates the aggressiveness of the lesion.
If the diagnosis of prostate cancer is confirmed, my practice is to go through the results with my patients patiently within the context of prostate cancer. It is important to reiterate that prostate cancer is a slow-growing cancer and that it becomes a team effort to overcome this challenge.
Team “We” (patients and I) can have discussions back and forth before deciding on a treatment course. Family members are invited to sit in at the next session with a list of written questions. There is no one-size-fits-all plan, as everyone is different.
Together with your PSA and biopsy grading, additional scans will be required to accurately ‘stage’ your scan. Staging is a necessary step in the management of cancers. It informs me of the degree of spread of the disease at the point of diagnosis. Staging is typically divided into stages 1 to 4. Stage 4 is the most advanced (the stage where sobbing in a drama starts).
There are a variety of treatments available in the armamentarium of a urologist when it comes to prostate cancer treatment. It can range from Active Surveillance to Robotic Surgery, from Watchful waiting to Palliative trans-urethral resection of the prostate (TURP).
The final decision is best appreciated through answering a 3-question rule-based approach.
- Does it need treatment?
- Is the treatment curative?
- Does the treatment outweigh the harm that the disease will likely post?
Only a limited permutation exists, and I will recommend the treatment plan to the patient, who makes the final decision based on his personal preference and beliefs.
The final decision is individualised and tailored to the person in front of me in consultation with the best available evidence-based medicine and the agreement of the patient’s loved ones. Regardless of the decision and outcome, my patient is guaranteed to have me walking their cancer journey together henceforth.
Article contributed by Dr Jay Lim Kheng Sit, Urologist, PanAsia
Surgery Group.
Dr Lim obtained his Bachelor of Computing from the National University of Singapore in 2005 and completed his graduate medical degree from the University of Sydney in 2009. He completed his Urology Surgical Training in 2017 and was interested in stone-related research, prevention and surgery. Dr Lim believes communication in English, Mandarin and dialects is critical to a robust Doctor-Patient relationship. A keen innovator, he was awarded the Singapore-MIT innovation fellowship in 2017. He is actively involved in the medical device innovation scene and holds a patent for his work.
Photo by Hush Naidoo Jade Photography and by Accuray on Unsplash