Insights + interviews
The role of healthcare practitioners in advocating cardiovascular health
This interview explores the link between cardiovascular health and nutrition, and the important role healthcare practitioners play in advocating cardiovascular health
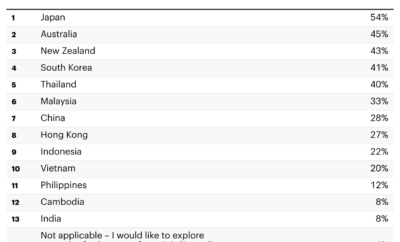
Cardiovascular disease is the leading cause of deaths worldwide, and half of the cases of cardiovascular diseases are estimated to be in Asia. According to the Singapore Heart Foundation, in 2020, cardiovascular disease accounted for almost 1 out of 3 deaths in Singapore.
We discuss the links between cardiovascular health and nutrition as well as the role healthcare practitioners (HCP) have in promoting good cardiovascular health to the communities they service with Dr. Simon Sum, Director, Scientific Affairs, Herbalife Nutrition.
the Active Age (AA): Can you share with us about what constitutes cardiovascular health?
Dr. Simon Sum (SS): Cardiovascular health constitutes the health of the heart and blood vessels. Common cardiovascular diseases (CVDs) that affect the heart and blood vessels include coronary heart disease, heart attack, and stroke, which are commonly caused by buildup of fatty deposits inside arteries.
We also see the rates of diabesity increasing (the term ‘diabesity’ is a convenient way of describing and discussing type 2 diabetes in the context of obesity). These two afflictions seem to converge and intersect more. Diabesity can also lead to the development and progression of CVD and hence, we should focus on factors affecting cardiovascular health.
AA: What are the links between cardiovascular health and nutrition?
SS: CVD has many risk factors, including high serum cholesterol levels, diabetes mellitus, obesity, tobacco usage, heavy alcohol use, and elevated blood pressure. The battle against CVD involves controlling its risk factors.
Most of these risk factors can be directly affected by the type of food one consumes.
The economic growth in Asian countries over the years has led to diet changes from healthier traditional diets to an overdependence on convenient/ fast-food diets that are calorie-dense and high in sodium, added sugar and saturated fats. Such diets aggravate risk factors and thus increase the risk of CVDs for Asians. We also know that Asian youths tend to prefer junk foods, which are usually missing the necessary nutrients like vitamins, minerals, and dietary fibres.
Therefore, for good heart health, it is crucial to consume a balanced diet aside from maintaining a healthy lifestyle with adequate exercise and proper sleep.
AA: Is there a particular diet or lifestyle nutrition model (e.g. intermittent fasting) that promotes good or better cardiovascular health?
People should avoid foods high in sodium, saturated and trans fats, salt, and added sugar, as they worsen risk factors of CVDs. They can instead opt for foods high in proteins, healthy unsaturated fats, dietary fibre, antioxidants, vitamins, and minerals, as these nutrients can be beneficial for heart health. Good examples of foods with a relatively high amount of healthy fats like omega-3 fatty acids include fish, seafood, and nuts.
Research has also shown that people who consume nuts regularly may be less likely to die from heart disease than those who rarely eat nuts.
We know that there are numerous benefits of eating more plant foods. Combining different plant foods in the diet can increase nutrient density, which means that they provide an abundance of nutrients relative to their calorie cost. Fruits, vegetables, beans, and whole grains are great sources of vitamins, minerals, and phytonutrients, and they’re naturally cholesterol-free.
In particular, Asian pears, citruses like pomelos, cruciferous vegetables such as Bok Choy, daikon, and green and yellow vegetables are effective for supporting good heart health.

Healthcare practitioners (HCPs) can educate their patients that switching to plant-based diets may not be intimidating. Small and simple ways can start with eating a fruit or ordering a vegetable dish with each meal and subsequently adding one or two vegetarian meals per week.
AA: Why does this diet work so well to protect or enhance cardiovascular health?
SS: Nutrient-dense foods help reduce CVD risk factors. Proteins help increase satiety, and are useful in managing weight, as well as obesity. Proteins also facilitates important bodily functions including muscle maintenance and repair, cell renewal, and wound healing, which are vital for good health.
In particular, research has found strong links between plant-based protein intake and lower overall mortality, as plant sources help providing a lot of nutrients including antioxidants and improving serum triglyceride and cholesterol levels, among many other benefits.
Also, unsaturated fats can improve blood triglyceride and cholesterol levels, ease inflammation and stabilize heart rhythms, among many other benefits. Finally, nutrients like fibers, vitamins and minerals can improve blood vessel function and help control obesity and diabetes.
AA: What is the link between COVID-19 and cardiovascular health? In particular, what is the impact on someone that has poor cardiovascular health contracting COVID-19?
SS: COVID-19 is a relatively new disease that is constantly changing. Its effects on cardiovascular health are not conclusive as these studies are still ongoing.
AA: What is the optimal role that a healthcare practitioner (HCP) plays when it comes to promoting or influencing cardiovascular health with their customer/community/patients?
SS: Having a reliable source of information is vital to build a strong foundation of knowledge on how to adopt diets that promote good heart health.
HCPs have been identified as the primary and most-trusted source of information people depend on for health-related issues. Therefore, the role of healthcare associations and HCPs is the key to influence patients to be mindful on what they consume to maintain their heart health.
Healthcare associations and HCPs can regularly incorporate the following actions in their practice:
- Implement a compulsory pre-consultation form in clinics for patients to indicate information regarding their health/ lifestyle habits. HCPs can use them to provide targeted recommendations accordingly.
- Remind patients that a heart-healthy diet does not only support heart health but also overall nutrition in various ways.
- Share with patients a list of convenient and nutritious foods and ingredients that are good for heart health.
- Encourage patients to avoid second-hand smoking. Non-smokers who have high blood pressure or high blood cholesterol have an even greater risk of developing heart disease when they’re exposed to second-hand smoke.
- Get patients to keep moving. Research has shown that staying seated for long periods of time is not good for overall health. Regular physical activity reduces the risk of having a heart attack or developing heart disease while helping to control risk factors like high blood pressure, high cholesterol, and obesity.
- Recommend important/credible channels that patients can use to receive accurate health-related information.
- Advocate the importance of reading food labels, using food tech like fitness and diet applications to improve patients’ heart health.

Overall, HCPs play a central and critical role in disseminating correct health-related information and educating patients about CVD.
Given the debilitating impacts of CVD on both individuals’ health and economies worldwide, particularly in Asia, HCPs’ intervention in the battle against CVD is essential. With adequate information, education and awareness, HCPs can effectively help reduce the incidence and prevalence of CVDs and enable people to lead healthier lives.
Photo by Iñigo De la Maza on Unsplash, by Febrian Zakaria on Unsplash and by Ali Hajiluyi on Unsplash